Our Orthopedic Anatomy Series takes you behind the procedure and explores what happens to your body before, during, and after treatment.
In the inaugural event of this ongoing series, we brought together OrthoCarolina shoulder surgeons and Experience Anatomy educators to present Exploring Your Body from the Inside Out – Shoulder edition. The physician panel dove into the anatomy of common shoulder injuries and treatments and answered audience questions in real-time.
Watch the Full Live Stream
The event took place on March 5, 2020, with audience members in attendance and was streamed live on Facebook and YouTube.
Featured Topics
- Shoulder Impingement & Rotator Cuff Tears
- Frozen Shoulder Treatment Options
- Shoulder Replacements: When & Why
Host
The event was hosted by Dr. Nady Hamid, MD, a shoulder & elbow surgeon with OrthoCarolina’s Shoulder & Elbow Center, South Park office and Sports Medicine Center.
Meet the Panel
Dr. Scott B. O’Neal, MD, is a shoulder & elbow, knee and sports medicine surgeon with OrthoCarolina Ballantyne.
Dr. Grant Mostak, MD, is a shoulder & elbow and sports medicine surgeon with OrthoCarolina Concord.
Dr. Shadley C. Schiffern, MD, is a shoulder & elbow surgeon with OrthoCarolina’s Shoulder & Elbow Center, South Park office and Sports Medicine Center.
Shoulder Impingement & Rotator Cuff Tears
Shoulder impingement typically is caused by compression of the rotator cuff. This pinching leads to bursitis and inflammation, which in turn can lead to partial rotator cuff tears. These partial tears can then lead to full thickness rotator cuff tears.
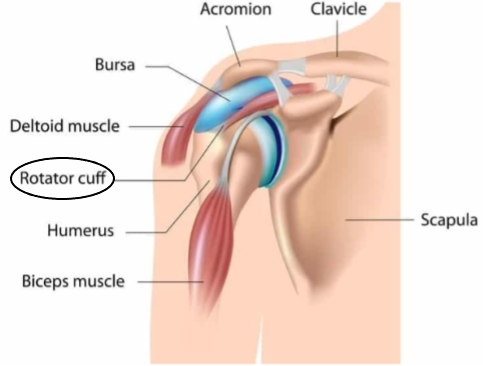
Symptoms include dull radiating pain, usually down the outside of the shoulder and stopping at the elbow. This pain may worsen with overhead activities and lessen with rest.
Treatment begins with conservative, non-surgical methods including nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin and ibuprofen, physical therapy, activity modifications and pain injections. When conservative options are not enough to manage pain and stiffness, your doctor may consider surgical options.
Frozen Shoulder
Frozen shoulder, or adhesive capsulitis, can describe multiple types of shoulder stiffness. It affects approximately two percent of the population, predominantly women ages 40 to 65.
Risk factors include diabetes, thyroid disease and autoimmune diseases.
Symptoms include pain at night and at rest, tenderness to touch at the front and back of the shoulder joint and reduced range of motion. Your doctor may conduct X-rays to rule out other causes of stiffness.
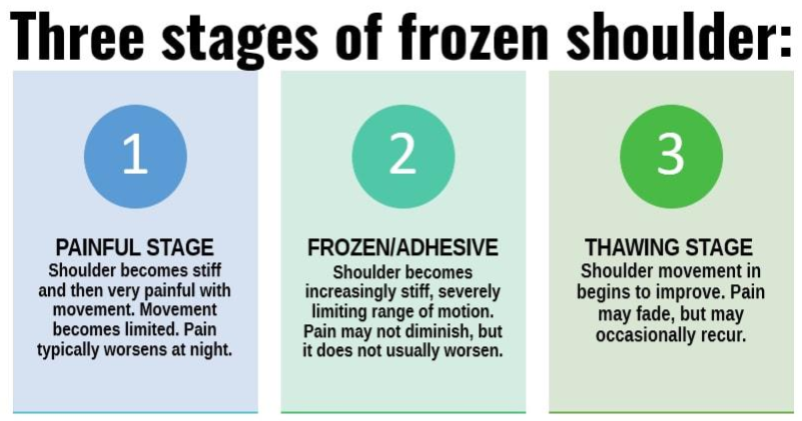
Three Stages of Frozen Shoulder
- Painful: Shoulder becomes stiff then very painful with movement. Movement becomes limited, and pain typically worsens at night.
- Frozen/Adhesive: Shoulder becomes stiff, severely limiting range of motion. Pain may not diminish, but it usually does not worsen.
- Thawing: Shoulder movement begins to improve. Pain may fade and occasionally recur.
Shoulder Replacements: When & Why
Two common types of shoulder replacement surgery are anatomic total shoulder arthroplasty and reverse total shoulder arthroplasty. Your doctor will determine which procedure is best for you based on diagnoses and presenting symptoms.
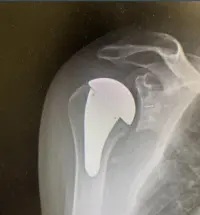
Anatomic Total Shoulder Arthroplasty
Common diagnoses include osteoarthritis of the glenohumeral joint, rheumatoid arthritis, avascular necrosis and post-traumatic arthritis.
Symptoms that indicate this surgery may be best for you include pain at night, stiffness, decreased mobility and crepitus, or cracking sounds, in the shoulder joint.
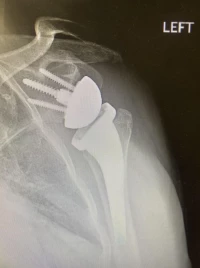
Reverse Total Shoulder Arthroplasty
Common diagnoses include massive, irreparable rotator cuff tears and rotator cuff tear arthropathy, or chronic rotator cuff tears with associated arthritis.
Symptoms that indicate this surgery may be best for you include pain at night, pain along the length of your arm, loss of function, weakness, and crepitus, or cracking sounds, in the shoulder joint.
Open Q&A

Our panel of experts concluded the event by answering audience questions during an open Q&A. Watch the complete Q&A discussion.
We're here to help you stay healthy, informed and uplifted as we navigate unprecedented change in our communities together.
Back



