Dr. Bryan M. Saltzman, MD
While many anterior cruciate ligament (ACL) injuries heal with time and proper rest, more severe ligament tears may need to be repaired surgically. ACL reconstruction surgery can help patients return to the sports and physical activities they love after a serious injury.
In part two of ACL Injuries 101, Dr. Bryan Saltzman, MD, explains when reconstruction surgery is the right choice and what to expect pre- and post-op. Dr. Saltzman specializes in cartilage restoration, adolescent and adult sports medicine, shoulder & elbow, and knee.
Sensitive content warning: This post contains images of surgical procedures.
Which patients are candidates for ACL reconstruction surgery?
Reconstruction surgery is not necessary for all ACL injuries and depends primarily on a patient’s individual goals. ACL reconstruction is not a time-sensitive procedure and can be performed electively unless there is urgent need to address greater damage to the cartilage, meniscus or other ligaments.
Unfortunately, the ACL cannot heal itself once torn. With that in mind, it is perfectly possible to live a healthy and functional life with a deficient ACL.
A functional ACL is not necessary for walking, standing, in-line running or taking stairs. Physical therapy, brace use and avoidance of cutting/pivoting activities may be treatment enough for older patients or patients who are disinterested in surgical options.
For patients who wish to return to exercise or sporting activities that use cutting, pivoting, twisting or lateral translation, surgical intervention is more appropriate as a first-line treatment. I recommend reconstruction surgery for these patients because further injury to the meniscus, cartilage or other ligaments can occur if the knee joint shifts without a functional ACL to protect and stabilize it.
How does a patient prepare for ACL reconstruction surgery?
Range of motion is the most important precursor to ACL reconstruction surgery. Stiffness prior to surgery leads to stiffness after surgery and can result in a less-than-optimal outcome.
For patients who have an ACL tear and no concurrent meniscus injury, I encourage them to continue to walk on the injured leg and move the affected knee to maintain mobility in the knee joint.
However, these patients should avoid any cutting, pivoting, twisting or lateral movements that could cause the knee to “shift.” Without the functional ACL present to stabilize the knee, shifting movements can lead to further injury.
For patients who have significant swelling or stiffness, I refer them to physical therapy for “pre-hab” to work on improving their range of motion and reducing fluid in the knee.
What is an ACL graft?
During reconstruction surgery, the surgeon removes the torn ACL and replaces it with a graft, or a portion of tissue used to make a new ligament. Once we determine reconstruction surgery is the most appropriate course of treatment, the patient and I will discuss which type of graft is the best for them.
There are two main graft options to reconstruct a new ACL: an allograft (or donor, cadaveric tissue) or an autograft (a portion of the patient’s own quadriceps tendon, hamstring tendon or patellar tendon).
How is ACL reconstruction surgery performed?
ACL reconstruction surgery is performed arthroscopically using a small camera and small instruments. The surgeon will draw the graft tissue across the knee joint and affix it to the femur (thigh bone) and tibia (shinbone) with a combination of suture, screws or buttons.
This procedure keeps the graft tissue taut and recreates the anatomy and biomechanical function of the ACL. Over time, the patient’s body will turn the reconstructed tendon into a new ligament.
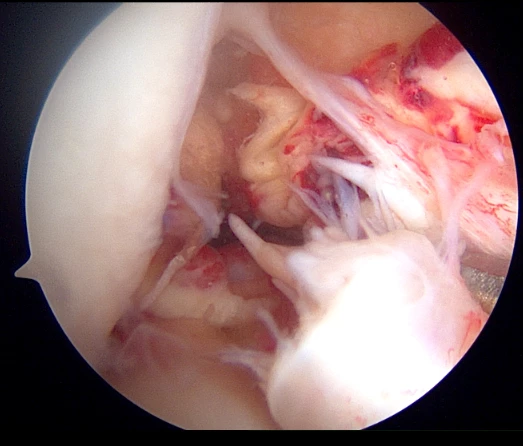
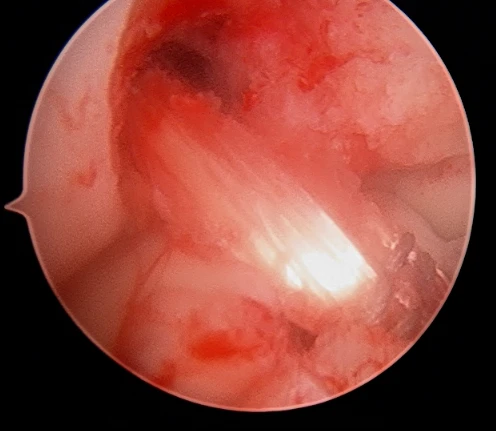
What is the recovery process like?
Although the rehabilitation process after ACL reconstruction surgery can be challenging, I remind my patients they will meet notable gains and benchmarks frequently along the way. Their physical therapist will become their new closest friend, as weekly therapy visits are necessary to progress through the rehab course.
Regaining full mobility of the affected knee is the early goal of rehabilitation efforts, and is imperative to a successful outcome. For this reason, I have my patients begin working on motion with their physical therapist by day three post-surgery.
If the ACL reconstruction is “isolated,” meaning no additional meniscus or ligament surgery was done, patients can typically bear full weight on the operative leg in a brace with crutches for assistance within the first week of surgery.
How long will it take A Patient to return to sports?
Here is a breakdown of the typical postoperative recovery from ACL reconstruction surgery.
- Initial weeks post-op: Focus on regaining motion and strengthening the quadriceps
- 6 weeks post-op: Discontinue use of a supportive brace, continue improving motion and gaining strength, begin using a stationary bike
- 3 months post-op: Begin using the elliptical
- 5 months post-op: Begin swimming and jogging
- 7 months post-op: Begin cutting/pivoting activities
- 9 months post-op: Return to sport
Fortunately, after the long rehabilitation efforts, the vast majority of patients regain full strength, motion and stability of the knee and can return to their sport of choice after ACL reconstructive efforts.
Dr. Bryan M. Saltzman, MD, is fellowship-trained in Shoulder & Elbow and Sports Medicine. He specializes in cartilage restoration as well as adolescent and adult sports medicine, shoulder & elbow and knee. He practices at OrthoCarolina's Cartilage Restoration Institute, Sports Medicine Center, and University office.
Back




