OrthoCarolina recently hosted a webinar answering common questions about hip replacement surgery, offering patients a deep dive into recovery, surgical options, and the latest technology in orthopedic care. Whether you’re considering a hip replacement or just researching your options, understanding what goes into a safe, successful procedure can help you make informed decisions.
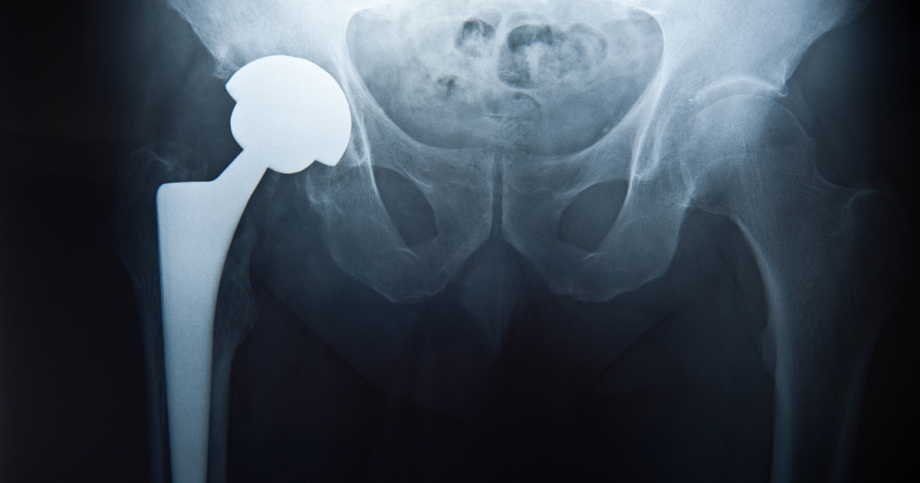
In this article, we’ll break down key insights shared by OrthoCarolina’s specialists Dr. Ellison and Dr. Kurkis, covering outpatient surgery, post-operative recovery, surgical precision, dual mobility implants, osteoporosis considerations, and when imaging is necessary before surgery.
Why Choose an Outpatient Hip Replacement?
Many patients are surprised to learn that hip replacement surgery doesn’t always require a hospital stay. At OrthoCarolina, our ambulatory surgery centers provide a high-quality, streamlined experience for joint replacement.
Benefits include:
- Lower cost: Outpatient centers can reduce the overall cost of care compared to inpatient hospitals.
- Specialized care: Surgery centers focus on orthopedic procedures every day, creating a consistent, efficient process.
- Better recovery experience: Patients often report smoother recovery due to fewer distractions and a more personalized environment.
Who is a candidate? Suitability depends on several factors, including age, medical conditions, baseline mobility, and home support. Your surgeon will help determine if outpatient surgery is the safest option for you.
Precision and Technology in Hip Replacement
Modern hip replacement isn’t just about replacing a worn joint; it’s about restoring proper function and reducing complications. Precision in component placement is critical for stability, range of motion, and recreating natural hip anatomy.
How surgeons ensure precision:
- Fluoroscopy: Real-time imaging allows for accurate positioning of the implant during surgery.
- Trial systems: Temporary implant placement helps make small adjustments before finalizing.
- Emerging technologies: Robotics, augmented reality, and AI can assist surgeons in achieving consistent results, though research is ongoing to confirm long-term benefits.
By leveraging these tools, surgeons can tailor each procedure to a patient’s unique anatomy, optimizing outcomes.
Choosing the Right Implant: Dual Mobility Hips
Some patients may benefit from dual mobility hip implants, which use a “ball within a ball” design to provide greater stability and range of motion.
How it works:
- A small ceramic ball attaches to the femoral stem.
- A larger polyethylene ball fits over the ceramic ball.
- The polyethylene ball sits within a metal hip socket.
Ideal candidates:
- Patients undergoing revision surgery or with prior soft tissue damage.
- Individuals recovering from hip fractures.
- Active patients with soft tissue laxity or those participating in activities requiring extreme hip mobility.
This design reduces the risk of dislocation and is particularly helpful for patients with higher instability risks.
Recovery After Hip Replacement
Recovery is a key concern for patients. While it varies by individual, OrthoCarolina surgeons emphasize early movement and gradual progression.
Post-operative guidelines:
- Walking: Most patients can safely walk the same day, with structured increases over time.
- Stairs: Patients can usually navigate stairs the same day if necessary, but repeated trips should be minimized in the first few days to reduce swelling and inflammation.
- Home setup: Consolidate your living space—keep essentials like your bedroom, restroom, and snacks nearby.
- Follow your rehab plan: Surgeons provide weekly activity progressions based on healing.
The goal is to regain mobility safely, while avoiding overexertion that could slow recovery.
Osteoporosis and Surgical Considerations
Bone health plays an important role in hip replacement planning. Osteoporosis, or reduced bone density, can influence implant choice and surgical technique.
What surgeons consider:
- Cemented femoral stems: Often used for patients with lower bone density for better stability.
- Press-fit hip sockets: Typically used even in patients with mild bone loss, allowing bone to grow into the implant over time.
- Surgical approach: Severe osteoporosis may influence the decision between anterior or posterior approaches.
Hip replacement addresses joint damage, not osteoporosis itself. Osteoporosis is usually managed medically through weight-bearing exercises, supplements, and medications to reduce fracture risk.
Imaging Before Surgery: X-rays vs. MRI
Most patients do not require an MRI before surgery. Plain X-rays usually provide sufficient information about arthritis severity and joint structure.
When MRI may be needed:
- Younger patients (<50s) with unexplained hip pain.
- Cases where X-rays do not show labral tears, avascular necrosis, or cartilage damage.
- Situations requiring more detailed planning for surgery.
Using imaging judiciously ensures surgeons have the information needed for safe, effective care without unnecessary tests.
Make an Informed Decision with OrthoCarolina
If you or a loved one are considering hip replacement surgery, trust OrthoCarolina for expert care and the latest in surgical technology. Our outpatient centers provide a streamlined, patient-focused experience, and our specialists will guide you through recovery, implant options, and post-operative care.
Schedule a consultation with OrthoCarolina today to learn which hip replacement options are right for you.
Frequently Asked Questions
Can I go up and down stairs immediately after surgery?
Yes, most patients can use stairs the same day. Limit trips in the first few days and follow guidance from your physical therapist to prevent swelling and pain.
What is a dual mobility hip replacement, and who needs it?
A dual mobility implant features a ball within a ball for greater stability. It is often used in revision surgeries, hip fractures, or for patients at higher risk of dislocation.
Does osteoporosis mean I need a different type of hip implant?
Possibly. Low bone density may require a cemented femoral stem for stability, but hip replacement is performed for joint damage, not as a treatment for osteoporosis alone.
Back



